Our Procedures
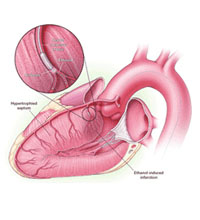
Alcohol Septal Ablation
What is an Alcohol Septal Ablation?
Alcohol septal ablation is often used instead of open heart surgery to treat patients with symptomatic hypertrophic obstructive cardiomyopathy. Dr Con Aroney pioneered this procedure in Queensland.
What is Hypertrophic Obstructive Cardiomyopathy?
It is a genetic condition, where an abnormal thickened ridge of heart muscle develops, and obstructs flow from the outflow tract of the heart’s main pumping chamber – the left ventricle. When the obstruction becomes severe, patients may develop shortness of breath, chest pain on exertion (angina) or blackouts.
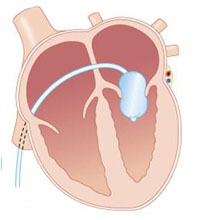
Mitral Ballon Valvuloplasty
What is an Mitral Ballon Valvuloplasty
The percutaneous treatment of symptomatic mitral stenosis was introduced to Queensland in 1990, by Dr Aroney, who has since performed over 300 procedures. He performs all his procedures at the Holy Spirit Northside Hospital, under local anaesthetic with sedation, through a puncture in the groin.
It has become the dominant primary mode of therapy for patients with symptomatic severe mitral stenosis, and is suitable for patients of all ages, including pregnant patients.
It is used for relief of symptoms (breathlessness) in patients with severe mitral stenosis.
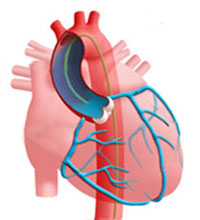
Coronary Angiogram
What is a Coronary Angiogram?
This procedure is performed to show any narrowing or blockage of your coronary arteries.
How is it done?The procedure begins with an injection of local anaesthetic, a fine tube (catheter) is put into the artery in the groin or arm. The tube is then passed into each coronary artery. A series of pictures are taken using X-Rays and a contrast medium (X-Ray dye).
Contrast medium is also injected into the main pumping chamber of the heart (left ventricle). This is used to measure the size of the heart and how well it is pumping.
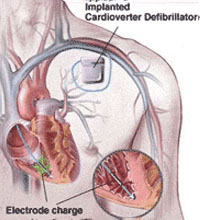
Defibrillator Implantation
When is a Defibrillator required?
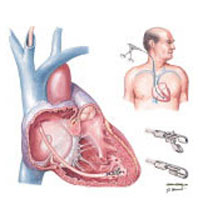
A major cause of death in the community is sudden cardiac death related to cardiac arrest. Cardiac arrest is generally caused with rapid ventricular tachycardia or ventricular fibrillation which leads to death within 5-10 minutes unless corrective action can be taken. Some of these cardiac arrests occur in patients who have had either previous heart attack but for a significant proportion it can be their initial presentation of their cardiac illness.
Drugs are only moderately effective at controlling this condition and generally patients who survive the cardiac arrest will need to have a device implanted which will be able to identify and then correctly treat the condition.
Endomyocardial Biopsy
What is an Endomyocardial Biopsy?
An endomyocardial biopsy is a procedure in which your doctor takes samples of heart tissue to help diagnose a number of cardiac conditions.
How is it done?The procedure begins with an injection of local anaesthetic into your right groin. A fine tube (catheter) is put into the vein in the groin. You may feel pressure in your leg while the tube is placed in the vein. The tube is passed up until it reaches the right heart chamber. This is painless. The doctor will use X-Ray images to see and guide the catheter.
Pacemaker Implantation
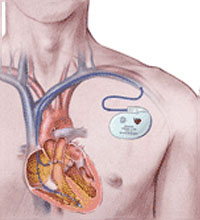
When is a Pacemaker required?
The normal heart beat is generated by the cardiac specialized conduction tissue known as the sinus node, also known as the intrinsic pacemaker of the heart. This cardiac tissue sometimes fails to generate a heart beat because of damage to that tissue through either inflammation, infection or generalised scarring.
The heart beat is then either extremely slow or fails to generate in which case the patient will feel extremely faint, dizzy and fatigued.
Radiofrequency Ablation
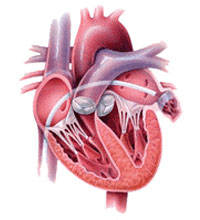
What is an Ablation?
In patients who are troubled by palpitations causing rapid heart rates a cardiac electrophysiology study is usually performed to determine the mechanism. Once the mechanism has been determined then the next method of curing the abnormal circuit is then contemplated.
How is it done?Most abnormal rhythms can be cured with a high degree of success (approximately 95%) using a specialized catheter which can be positioned at the site of the abnormality and then using radiofrequency energy the distal electrode tip of that catheter can be heated up to 65°C and with that will cause a 5mm scar at the site of the abnormal focus and will ablate the electrical activity and arrhythmogenic potential of that focus which will heal into a dense scar.
Transcutaneous Ablation of Septal Hypertrophy
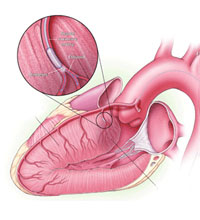
What is an Transcutaneous Ablation of Septal Hypertrophy
Patients with hypertrophic obstructive cardiomyopathy have abnormally thickened walls of the the left ventricle, the heart’s main pumping chamber. The interventricular septum — the wall of muscle between the two ventricles of the heart — is often excessively thickened. This thickened wall can interfere with the function of the mitral valve and can block the flow of blood out of the heart. The inefficient blood flow causes the pressure in the heart to increase, making the left ventricle work harder, resulting in further thickening of the walls of the left ventricle over time. Symptoms associated with HOCM can include chest pain, shortness of breath, palpitations, syncope (sudden fainting), and even sudden death.
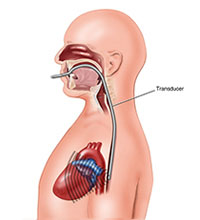
Transeosophageal Echocardiogram
What is a Transoesophageal Echocardiogram?
A Transoesophageal Echo (TOE) is an ultrasound examination that produces detailed pictures of your heart. The test is performed by the cardiologist (heart specialist) with the assistance of an anaesthetist (doctor specializing in anaesthesia) and nursing staff.
How do I prepare for it?
- No food or drink for 6 hours before the test (medications may be taken with sips of water).
- Please ensure that somebody accompanies you to the test as you will be unable to drive for the remainder of the day (because of sedation).
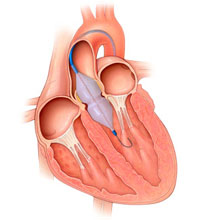
Aortic Ballon Valvuloplasty
What is a Aortic Ballon Valvuloplasty
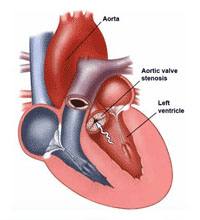
Percutaneous aortic balloon valvuloplasty (PABV) is used to relieve severe obstruction of aortic valve stenosis, which causes shortness of breath, chest pain or blackouts. It carries a significantly lower risk than surgical aortic valve replacement (being performed whilst teh patient is awake under local anaesthetic, through a puncture in the groin), but there is less clinical improvement after the procedure and benefits are sustained for a shorter period, usually for about 12 months. Therefore, the procedure is recommended for patients who are not candidates for valve surgery. Patients are hospitalized for only one or two days after the procedure.
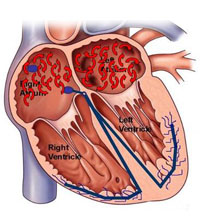
Cardioversion
What is a Cardioversion?
Elective cardioversion is usually performed for arrhythmias of the heart such as atrial fibrillation or flutter. Using sedation under the supervision of an anaethetist, one of our Cardiologists gives your heart an electrical shock to restore normal heart rhythm
How do I prepare for it?You should fast for 6 hours prior to the procedure and take your usual medications as directed by your specialist. You will be admitted to the hospital as a day patient.

Coronary Angioplasty and Stenting
What is Angioplasty and Stenting?
Angioplasty and stenting is often used instead of surgery to treat narrowed or blocked coronary arteries.
How is it done?The procedure begins with an injection of local anaesthetic in the groin/arm, a fine tube (catheter) is put into the artery in that location. The tube is passed into the coronary arteries. A series of pictures are taken using X-Rays and X-Ray dye. If any narrowing or blockages are found then a tube with a tiny wire is passed down the affected artery so that a sausage-shaped balloon can be passed over it and into the part that is narrowed or blocked.
To open up the artery, the balloon is blown up with fluid, which then presses against the cholesterol plaque. pushing it out of the way.
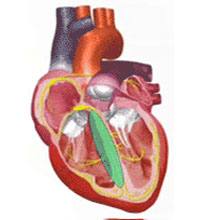
Cardiac Electrophysiology Study
What is a Cardiac Electrophysiology Study?
A cardiac electrophysiology study is a study performed by a Heart Specialist with specialized training in abnormal rhythms of the heart. To have this study performed you would need to be admitted to a hospital with specialized equipment necessary to perform this procedure. You will generally be admitted on the day of the procedure and will need to fast for 3-4 hours prior to the procedure.
How is it done?The procedure is performed using local anaesthesia with IV sedation which will be given in doses requisite to make you feel calm and slightly sleepy but you will not be rendered unconscious. Small plastic tubes will be placed in the veins of the leg or arm. Through these tubes insulated wires or catheters are placed through the veins into the heart.
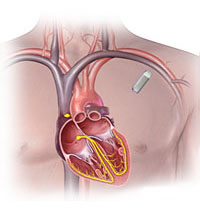
Implantable Loop Recorder
What is an implantable Loop Recorder?
In patients who have very infrequent symptoms of palpitations or dizziness and fainting, where the standard electrocardiogram and Holter monitor has failed to yield the cause for the problem, the patient can then be fitted with a device called an implantable loop recorder.
How is it done?This device is implanted beneath the skin on the anterior chest wall to the left of the breast bone. This location yields the best site to record the cardiac electrical activity. The loop recorder will continuously monitor the heart rhythm and automatically record any abnormal rhythms.
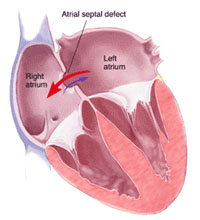
Percutaneous Closure of Atrial Septal Defect and Patent Foremen Ovale
What is Atrial Septal Defect (ASD)?
An ASD is a congenital defect (present from birth) where a hole is present between two chambers of the heart: the left and right atria. This leads to an abnormal flow of blood from the left heart into the right heart, which leads to increasing strain on the right heart, which can damage the right side of the heart and lead to “cardiac failure” and palpitations..
What is a Patent Foramen Ovale (PFO)?A PFO is “flap valve” communication between two chambers of the heart (the left and right atria) which usually closes after birth, but which can remain open into adulthood. This communication increases the likelihood of a person having a stroke, transient ischemic attack (TIA ) or systemic embolus, by allowing clots to pass from the venous circulation into the systemic arterial circulation and into the brain or elsewhere. Patients with PFO also have an increased prevalence of migraine.
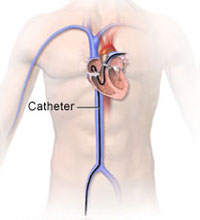
Right Heart Catheter
What is a Right Heart Catheter?
This is a procedure where catheters are passed into the arteries and veins of the heart. Heart and lung pressures are monitored and blood samples are taken from within the heart.
How is it done?The procedure begins with a tube (catheter) being put into the vein in the groin. You may feel pressure in your leg while the tube is placed in the vein. It is passed along until it reaches the heart and then goes up into the blood vessels of the lungs. This is painless. The doctor uses X-Ray imaging to see the catheter.
Transcutaneous Aortic Valve Implantation TAVI
What is a Transcutaneous Aortic Valve Implantation?
TAVI is the implantation of a bioprosthetic (pig or beef) aortic valve into a patient with severe aortic valve disease.
Two types of valve are being implanted:
• Medtronic Corevalve
• Edwards Valve
Dr Darren Walters and Dr Con Aroney pioneered these procedures in Queensland.
Transthoracic Echocardiogram
What is a Transthoracic Echocardiogram
A transthoracic echocardiogram is a test that takes images of the heart with the use of a transducer (probe) placed on the chest wall. Harmless ultrasound technology is used. High frequency sound waves inaudible to the human ear are sent from the probe and directed toward the heart. As the sound goes through the different structures, part of it bounces (echoes) back to the probe and is interpreted by the ultrasound machine into images of the beating heart. The images are then displayed on the monitor and recorded for future review
At Queensland Cardiology, the test is performed by a sonographer trained in cardiac ultrasound and is interpreted by a Cardiologist.
